Comprehensive Overview of the Reproductive System
Introduction
In this study, the structure and function of male and female reproductive system us to be discussed. Moreover, the role of hormones at different stages from gametogenesis to menopause along with the process or sequences present from fertilisation to childbirth are to be discussed. For those seeking biomedical science dissertation help, understanding these aspects thoroughly is essential. In addition, the function of the placenta in pregnancy is to be discussed
Structure and function of male and female reproductive system
The external parts of the male reproductive system are penis which is elongated tube-like organ containing different parts that is root, body or shaft and glans that is the cone-shaped part of the organ. The urethra which is responsible for passing semen and urine is located at the tip of the penis. The function of the penis is to transfer semen that contains sperm during the sexual intercourse in the vagina of the female (Schlegel and Katzovitz, 2020). The other parts include scrotum which is pouch-like lose sac of the skin hangs from behind the penis and holds testicles. Its key function is to protect the testicles (Radke et al., 2018). The internal part of the male reproductive system are vas deferns which is an elongated muscular tube initiating from epididymis to pelvic cavity and its function to transport majored sperm to the urethra for it to be transported during ejaculation (Knoblaugh et al., 2018). The ejaculatory duct is developed with the fusion of seminal vesicles and vas deferens which end in the urethra. The urethra is the tube connecting the bladder to the outside and it functions to expel semen during ejaculation as well as acts in passage of urine (Joseph and Vezina, 2018). The seminal vesicles functions to produce most of the ejaculatory fluid and prostate gland acts in nourishing the sperm which is produced by the testicles within the seminiferous tubules (Knoblaugh et al., 2018).
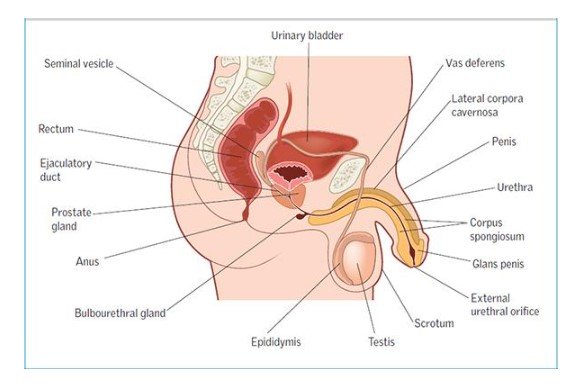
The external parts of female reproductive system include labia majora and minora which are large and small lips enclosing and protecting the other external reproductive organs. During puberty, the labia major support growth of public hair from its skin and contains oil and sweat secreting glands. The Bartholin glands are present near the vaginal opening on the either side of the vagina and produces mucus. The clitoris is the part where two labia minora meets and it is a sensitive part which is covered by prepuce similar to the foreskin of the penis (Christena, 2018). The internal organs initially include vagina that is the opening canal joining the cervix outside the body and acts as passage for entry of the penis along with function as release canal for the baby during birth (Cunha et al., 2018). The other internal organ includes uterus which is a hollow and pear-shaped organ functioning as the place for development of foetus. During each menstrual cycle, the endometrium grows on the wall of the uterine muscles inside the uterus and at the end of the menstruation, the canal in the end allow the menstrual blood to flow out. The ovaries are other internal organ that functions to produce eggs and hormones like progesterone and oestrogen. The fallopian tubes are narrow tubes attached at the upper region of the uterus and it functions to allow eggs from the ovary to travel to the uterus for it to be fertilised by the sperm for its implantation in the uterus (Robboy et al., 2017).

Role of hormones in developmental stages
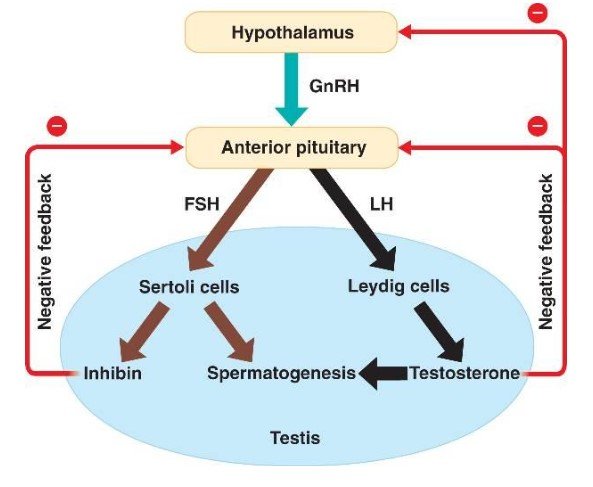
Gametogenesis: The gametogenesis is the process in which the haploid or diploid precursor cells are seen to undergo cell division to form mature haploid gametes and the two form of gametogenesis are spermatogenesis and oogenesis. The Follicle-Stimulating hormone (FSH) and the Luteinising Hormone (LH) are pituitary gonadotropins that are responsible in spermatogenesis. In spermatogenesis, the FSH acts to stimulate the production of ABP (androgen binding protein) from the Sertoli cells and allows formation of blood-testes barrier which functions in sequestering germ cells for its completion of meiosis (Javed and Al Sufyan, 2019). In the presence of LH, the Leydig cells stimulates formation of testosterone which regulates the spermatogenesis process. The inhibin acts in lowering the level of FSH and LH and when they are extremely lowered the testosterone level is lowering that sends signals to the pituitary for its further secretion. Thus, LH mainly secrets Leydig T cell and FSH stimulates Sertoli cell that occur in synergy with the T cell production and acts in maintaining spermatogenesis (Zhou et al., 2019).
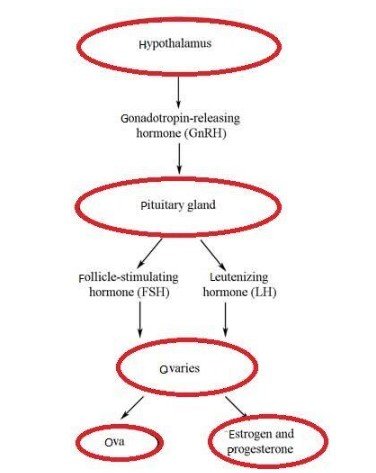
In case of females, the FSH acts in stimulating the eggs cells known as ova that later develops within the follicles. The inhibin is produced from the follicular cells and acts in inhibiting FSH after the release of the egg. LH additionally plays their part in development of ova by inducing it and stimulating progesterone and oestradiol that helps in preparing the body to be pregnant (Marques et al., 2020
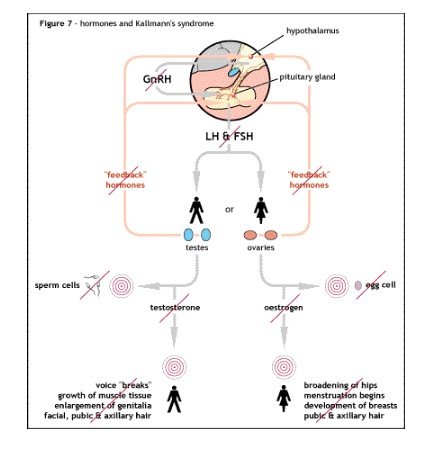
Puberty: The development of puberty occurs with the part of the brain that is hypothalamus initiating to produce hormone name gonadotropin which has impact on the ovaries and testis along with increases the production of sex hormones that are testosterone in boys and oestrogen in girls (Guo et al., 2020). The oestrogen along with FSH and LH during puberty in girls leads to initiate menstrual cycle along with formation of pubic hair and other maturity in the body features such as formation of breasts (Avendaño et al., 2017). In puberty, the testosterone plays the role of development of male features such as beard, deeper voice, body hair and others along with promotes body mass and sex drive.
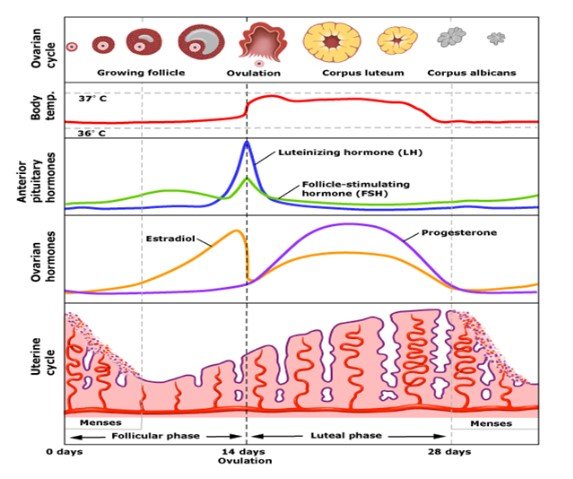
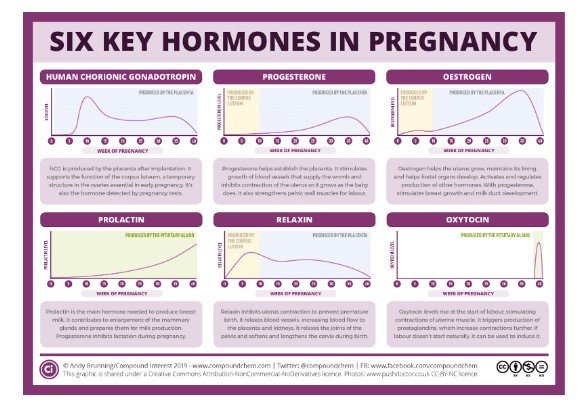
Pregnant: The role of hormones in pregnancy such as human chronic gonadotropin hormone (hCG) which is made only during pregnancy include to promote secretion of progesterone by the corpus luteal cells, angiogenesis development in the uterine vasculature, fusion and differentiation of cytotrophoblast cell un forming syncytiotrophoblast cells which helps to block any macrophage who are trying to invade the placental cells (Peng et al., 2021). The other hormone includes human placental lactogen (hPL) that acts in simulating the milk glands in the breast, oestrogen that takes part in formation of placenta during the pregnancy and progesterone that act in thickening the uterine lining for implanting the fertilised egg (Velegrakis et al., 2017)
Menopause: During menopause, the ovaries release less amount of estrogen that plays the role of decreasing and irregulating the menstrual cycle, in turn, leading it to be stopped. The formation of progesterone is also stopped and the testosterone level in the males are weakened but not entirely stopped (Stuenkel, 2017).
Process and sequences of events during fertilisation, implantation, foetal development and childbirth
The fertilisation process initiates from the sperm being ejaculated in the vagina where it undergoes capacitation through intracellular increase of calcium ions, increased spermatic motility and loss of surface antigens that renders it to be actively receptive to penetrate the egg (Bianchi and Wright, 2020). The following step is sperm-egg binding which occurs with the sperm binding to the zona pellucida of the egg which is triggered by the appropriate presence of glycoprotein on the surface of the sperm. The binding triggers the acrosomal reaction where the enzyme of the acrosome is freed and the zona pellucida gets digested to allow the sperm to move towards the plasma membrane of the egg (Hamze et al., 2019). The next stage is sperm-egg fusion in which the sperm on entering the egg move by penetrating its plasma membrane towards the nucleus and fusion of both the nucleus of sperm and egg occurs to finally fertile the egg (Hamze et al., 2019).
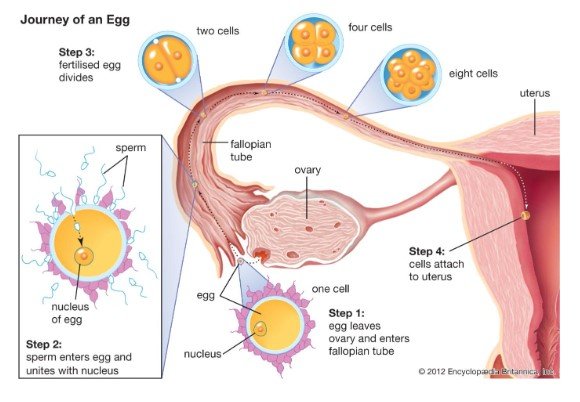
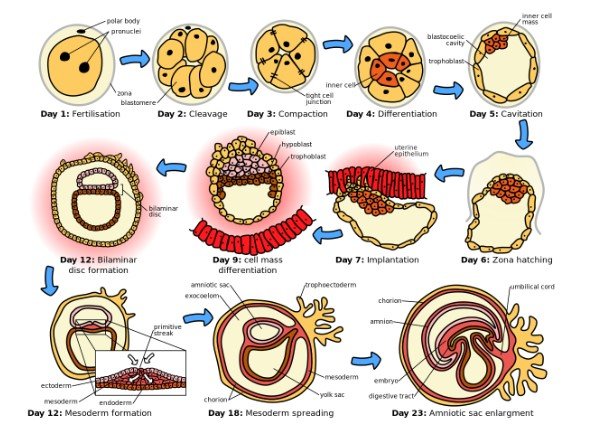
The process and sequence of implantation of the fertilised egg initiates with the apposition of blastocysts at the uterine epithelium which is the site connecting with the implanted site of the endometrium. It is followed by formation of trophoblast cells of the blastocyst that attaches with the receptive endometrial epithelium by migrating deep into the maternal decidua. Finally, the invasive trophoblast cells are formed that cross the endometrial epithelial basement membrane and invade the stroma of the endometrium with the process known as invasion (Zhou et al., 2019)
The foetal development consists of three stages that are first trimester, second trimester and third trimester. In the first trimester, the fertilised egg initiates to become an embryo which is made up of three layers of tissue with the inner layer to be dived into lungs, digestive system and liver of the baby (babycentre.co.uk, 2019). The second layer develops to become the bone, heart, kidney and sex organs and the outer layers initiates to become skin, eyes, hair and nervous system. In this phase, through cell division the heart, brain and lungs develop rapidly and around 6 weeks their heart initiate to beat. The embryo takes in nutrient and release waste through the umbilical cord (babycentre.co.uk, 2019). In the second trimester, the baby’s hair and eyebrows initiate to grow along with their muscle and bone. In this stage, if the baby is female, her eggs initiate to develop along with her ovaries. In the third trimester, all the parts of the baby is fully grown and they show ability to hear sound and respond to voices through movement within the uterus (babycentre.co.uk, 2019)
The process and sequence of childbirth includes four stages which are first, second, third and fourth stage of labour. In the first stage, the contraction of the cervix initiates which makes it to become thin and open with the process knowing as effacement and dilation. As the dilation of the cervix get completed, the baby birth occurs with simultaneously contraction of the uterus to push the baby to be released. In the third stage of labour, the baby is pushed out and the uterus continues to contract for pushing out the placenta. The fourth stage is the end of childbirth where the baby with the placenta is released out and the cervix is contracted (Slade et al., 2019).
Explanation of placental function during pregnancy
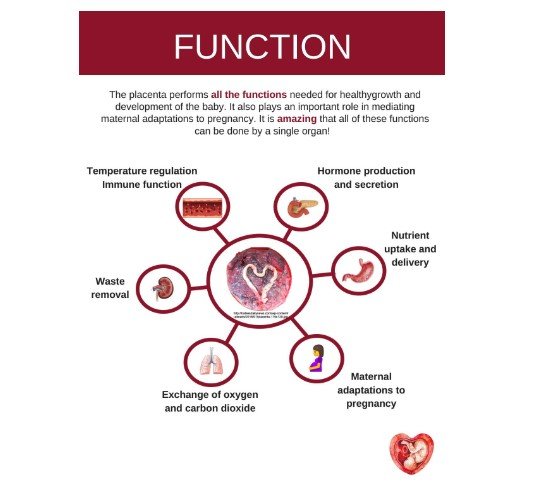
The function of the placenta during pregnancy includes supporting respiration, excretion, delivery of nutrition, supporting immunological functioning and acting as endocrine barrier. The other function includes clearing out the waste products from the embryo along with metabolising and releasing food substances along with needed product into the foetal and maternal blood circulations. The protection of embryo or foetus from xenobiotics, helping in formation of peptide and steroid hormones, protection of foetus from bacterial infection and others, protection from transfer of noxious substances and formation of enzymes like oxytocinase and diamine oxidase is supported by the placenta during pregnancy (Richard et al., 2017).
Conclusion
The above discussion informs that both male and female have external and internal reproductive organ that help in copulating and reproducing through transfer of sperm from the male to the female. The follicle-stimulating hormone, luteinising hormones along with progesterone and oestrogen in female and testosterone in male are involved at different developmental stages from gametogenesis to menopause. The fertilisation of the egg followed by implantation in the uterus gradually leads towards formation of the baby. The placenta play a key role in pregnancy by allowing transfer of nutrients, release of waste products, allowing respiration and others between the mother and the baby.
Recommendations
The above discussion leads to the recommendation that LH and FSH are required to be appropriately controlled as they are key hormones that allows initiation of spermatogenesis and plays active part in puberty. The other recommendation is that people are to be educated regarding the minute process extending from fertilisation to childbirth so that they are able to keep control of their health to support the smooth progress of the process and sequence of actions in the body.
Continue your journey with our comprehensive guide to Cellular Protein Isolation And Analysis.
References
Avendaño, M.S., Vazquez, M.J. and Tena-Sempere, M., 2017. Disentangling puberty: novel neuroendocrine pathways and mechanisms for the control of mammalian puberty. Human reproduction update, 23(6), pp.737-763.
babycentre.co.uk 2019, Foetal development week by week, Available at: https://www.babycentre.co.uk/pregnancy-week-by-week [Accessed on: 8 February 2021
Bianchi, E. and Wright, G.J., 2020. Find and fuse: Unsolved mysteries in sperm–egg recognition. Plos Biology, 18(11), p.e3000953
Christena, P., 2018. Anatomy and physiology of the female reproductive system. TNNMC Journal of Obstetrics and Gynaecological Nursing, 6(2), pp.46-46
Cunha, G.R., Robboy, S.J., Kurita, T., Isaacson, D., Shen, J., Cao, M. and Baskin, L.S., 2018. Development of the human female reproductive tract. Differentiation, 103, pp.46-65.
Guo, J., Nie, X., Giebler, M., Mlcochova, H., Wang, Y., Grow, E.J., Kim, R., Tharmalingam, M., Matilionyte, G., Lindskog, C. and Carrell, D.T., 2020. The dynamic transcriptional cell atlas of testis development during human puberty. Cell stem cell, 26(2), pp.262-276.
Hamze, J.G., Canha-Gouveia, A., Algarra, B., Gómez-Torres, M.J., Olivares, M.C., Romar, R. and Jiménez-Movilla, M., 2019. Mammalian spermatozoa and cumulus cells bind to a 3D model generated by recombinant zona pellucida protein-coated beads. Scientific reports, 9(1), pp.1-12.
Javed, M. and Al Sufyan, H., 2019. Spermatogenesis why some treatments or conditions make men infertile. Advances in Reproductive Sciences, Reproductive Health & Infertility.pp.89-111.
Joseph, D.B. and Vezina, C.M., 2018. Male Reproductive Tract. Encyclopedia of Reproduction, p.248.
Knoblaugh, S.E., True, L., Tretiakova, M. and Hukkanen, R.R., 2018. Male reproductive system. In Comparative Anatomy and Histology (pp. 335-363). Academic Press.
Marques, B., Matos, R. and Martinho, R.G., 2020. Oogenesis Signaling from Development to Environmental Plasticity and Aging. In Tissue-Specific Cell Signaling (pp. 317-335). Springer, Cham.
socratic.org 2018, hormones that regulate the menstrual cycle, https://socratic.org/questions/what-are-the-four-hormones-that-regulate-the-menstrual-cycle-thanks [Accessed on: 17 February 2021]
Peng, J., Liu, L., Feng, S. and Xing, N., 2021. Lung neoplasm mimicking as ectopic pregnancy due to paraneoplastic secretion of human chorionic gonadotropin: a case report and literature review. Archives of gynecology and obstetrics, pp.1-8
Radke, E.G., Braun, J.M., Meeker, J.D. and Cooper, G.S., 2018. Phthalate exposure and male reproductive outcomes: A systematic review of the human epidemiological evidence. Environment international, 121, pp.764-793.
Richard, K., Holland, O., Landers, K., Vanderlelie, J.J., Hofstee, P., Cuffe, J.S. and Perkins, A.V., 2017. Effects of maternal micronutrient supplementation on placental function. Placenta, 54, pp.38-44.
Robboy, S.J., Kurita, T., Baskin, L. and Cunha, G.R., 2017. New insights into human female reproductive tract development. Differentiation, 97, pp.9-22.
Schlegel, P.N. and Katzovitz, M.A., 2020. Male reproductive physiology. In Urologic Principles and Practice (pp. 41-62). Springer, Cham.
Slade, P., Balling, K., Sheen, K. and Houghton, G., 2019. Establishing a valid construct of fear of childbirth: findings from in-depth interviews with women and midwives. BMC pregnancy and childbirth, 19(1), pp.1-12.
Stuenkel, C.A., 2017. Menopause, hormone therapy and diabetes. Climacteric, 20(1), pp.11-21.
Velegrakis, A., Sfakiotaki, M. and Sifakis, S., 2017. Human placental growth hormone in normal and abnormal fetal growth. Biomedical reports, 7(2), pp.115-122.
Zhou, R., Wu, J., Liu, B., Jiang, Y., Chen, W., Li, J., He, Q. and He, Z., 2019. The roles and mechanisms of Leydig cells and myoid cells in regulating spermatogenesis. Cellular and Molecular Life Sciences, 76(14), pp.2681-2695.
Zhou, F., Wang, R., Yuan, P., Ren, Y., Mao, Y., Li, R., Lian, Y., Li, J., Wen, L., Yan, L. and Qiao, J., 2019. Reconstituting the transcriptome and DNA methylome landscapes of human implantation. Nature, 572(7771), pp.660-664.
Bibliography
Adah, A.S., Adah, D.I., Biobaku, K.T. and Adeyemi, A.B., 2018. Effects of Electromagnetic radiations on the male reproductive system. Anatomy Journal of Africa, 7(1), pp.1152-1161.
Arbib, N., Hadar, E., Sneh-Arbib, O., Chen, R., Wiznitzer, A. and Gabbay-Benziv, R., 2017. First trimester thyroid stimulating hormone as an independent risk factor for adverse pregnancy outcome. The Journal of Maternal-Fetal & Neonatal Medicine, 30(18), pp.2174-2178.
Stirrat, L.I., Walker, J.J., Stryjakowska, K., Jones, N., Homer, N.Z., Andrew, R., Norman, J.E., Lightman, S.L. and Reynolds, R.M., 2018. Pulsatility of glucocorticoid hormones in pregnancy: changes with gestation and obesity. Clinical endocrinology, 88(4), pp.592-600.
van der Giessen, J., van der Woude, C.J., Peppelenbosch, M.P. and Fuhler, G.M., 2019. A direct effect of sex hormones on epithelial barrier function in inflammatory bowel disease models. Cells, 8(3), p.261.
- 24/7 Customer Support
- 100% Customer Satisfaction
- No Privacy Violation
- Quick Services
- Subject Experts



