Analyzing Healthcare Financing in South Sudan
1. Key features of the health system component
Here, the focus on the component is identified in terms of financing. In South Sudan, it is one of the most important components in healthcare to focus on financing. The country usually spends a large amount on healthcare. The data relating to lower-income countries shows that a predominance of out-of-pocket payments is defined as a source of funding. Public financing requires the governments and other official actor involvement (Bilali, 2020). The out-of-pocket payments are regressive as they are done with exact market prices and are determined by the interaction of demand and supply. A lack of payment ability by the patients generates financial barriers to healthcare. This situation highlights the need for healthcare dissertation help to explore alternative funding models. Financing healthcare in this way implies that the cost of a household is being extremely volatile.

Additional healthcare costs might impact the household as the budgets are catastrophic and the additional cost of healthcare impacts the family's standard of living. "South Sudan healthcare spending for 2018 was $27, a 1.53% increase from 2017 (Hassan, Tudor, and Vaccari, 2018). South Sudan healthcare spending for 2017 was $26” (Who.int, 2021). The federal and health military services, universities, policies, and private sectors pay for healthcare in Sudan.
Before the 1990's the care recipients at public healthcare facilities were mostly free, however, some structural reformation introduced in 1992 aligned users with fees. The majority of the health services are accessible freely to the primary and secondary levels of the population (world bank, 2021). Still, the poor access to healthcare benefits had shown 96 deaths per 1000 childbirths (Who.int, 2021). The number of hospitals is less as it is 272 in 2019 as compared to the population of 13 million. Moreover, physicians reported 0.2618 in number per 1000 people whereas the number of community midwives is less than 100 as per the reports (Hassan, Tudor, and Vaccari, 2018). Meager income and difficult working conditions give limited career options to them while making the process of healthcare difficult. In September 2020, the World Bank approved 21.99 million to help the Sudan healthcare system and aided the fundraiser (world bank, 2021). The basis of contribution in money pooling can come from different aspects which are private insurance, social insurance, and taxation. Payment of premiums with an exact plan to contribute to healthcare works to a large extent in extensive healthcare threat management.
The process of money pooling is associated with insurance markets. There is the uncertainty generated across individuals of the society (Bilali, 2020). Health insurance has been seen to pool the risk of uncertainty across individuals. People are seen to have fallen sick within the specified period while others will not. The issue is to smoothen the pooling of risk between poor and non-poor so that the healthcare will be managed or through prepayment. Moreover, there is a significant threat of overconsumption observed that is found to be expensive in forms of healthcare (Salim, and Hamed, 2018). In public health, people want to have insurance coverage while they want to ensure the management of financial coverage. From a broader perspective of social welfare, the people will be capable of managing and allocating resources. The ability to pay and process healthcare security is important. Some people might not choose to buy health insurance. This occurs due to different misconceptions and staying indifferent towards the moral hazards (Adwok et al. 2019). The progressive improvement of individuals process on the income distribution and raises a fixed cost proportional management. Vertical equity is associated with insurance procedures depending on income status. There are horizontal equity observed that are regressive and expenditures are given high priority. In the private healthcare system, there are higher chances of operational changes observed.
2. Assessing the performance of specified components
This section of the study talks about the performance of financing as a health component and talks about health policy objectives, such as equity, efficiency, quality.
Equity: people these days are focused on equity of healthcare coverage. Market failures and adverse selections are seen not to be providing equity of coverage and that too while public health and welfare is taking appropriate actions (Salim, and Hamed, 2018). Markets are seen to be achieving even more pay that is progressive which is proportional and allocated to the fixed income distribution components. Equity financing is experienced in terms of the insurance market where people are allowed to be paid based on risks (Adwok et al. 2019). There is vertical equity observed that shows a different income status and concerns with horizontal equity which significantly differs from a position of health insurance activation. Private insurance in health is often seen not to be related to vertical or horizontal equity. Now, these two terms can be defined as a method of collecting income tax in which the tax paid has increased the people supposed to be contributing more rather than the ones that have not in vertical equity. Whereas, in horizontal equity the payers are supposed to be paying equal income tax and obligation might vary
Efficiency: the efficiency in objectives in the health sector is processing the equity achievement and managing the high premium which is out of reach of many. Efficiency objectives in health care talk about experience rating and adjusting the premium by expected losses in the policy which has been designed. Higher costs and higher premiums are seen to be due to finding of the loss that is fixed such as a job that an actor can control (Salim, and Hamed, 2018). High-tech diagnostic or curative interventions are seen to be much more profitable as they might result in non-price competition and allocate resources on the total management of moral hazards.
Quality: Quality of healthcare is largely associated with the performance management of each related to healthcare components. All nurses, doctors need to perform their routine duties to ensure that each individual is covered under health security (Kheder, Awad, and Hamid, 2020). Quality healthcare goals are found to be spending less at the time of fatal hazards. Paying previously and managing each insurance is associated with the client's performance and action-taking process. The adverse selection and moral hazard management lie within information handling threats. From a broader perspective of social welfare, it is important to take control of a marketing system. The marketing system might find moral hazard reporting as an additional burden. However, it will be managed anytime sooner with buying efficient products. Amplifying this problem associate equity coverage and seeking and advocating permission on income distribution. The proportion of income allocated to health might be reduced with a regressive financing mechanism and it needs to be changed on an immediate basis.
Medicare and Medicaid are associated with healthcare financing components at their best. Higher-income rates and less impact of taxes on essential commodities such as cigarettes tend to be regressive. Governments are operating on the fixed percentages of payment ability and social insurance coverage is improvised (Kheder, Awad, and Hamid, 2020). A high rate of financing components processes the redistribution factors of being healthy and sick both within rich and poor. Constrained by the available government resources sometimes become the main reason for not being able to work on global health issues. Substantial reliance on public financing has components such as citizenship and residual health benefits management system. All these progressive components need to be powered with adequate resources and control the public financing process.
3. Variables accountable for the level of performance which is observed
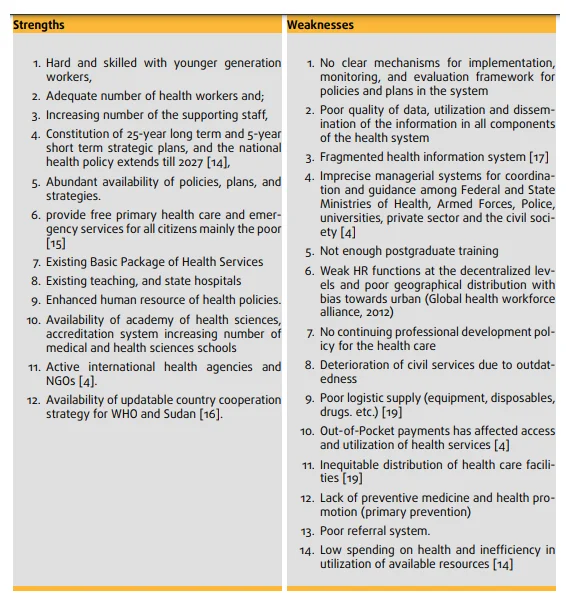
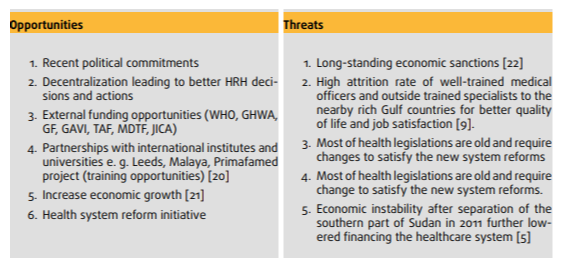
Variables that are accountable for the level of performance in health financing systems are found to be labor market shortage and unequal pay. Inadequacy of the payment systems has been focusing on the non-equal distribution of resources. No equal process of financing targets healthcare at the first and foremost level (Lohiniva et al. 2021). The labor market shortage in healthcare is being a primary reason that works as a threat of healthcare degradation. Trained HRH is less in number and a huge shortage of rehabilitation of healthcare and training schools are contributing to it. Unskilled professionals in any sector become a huge cause of the labor distribution threat. The impact of unfavorable working conditions gives them a threat to them so that they are not interested in the selfless care of the patients anymore.
HIV and other viruses that are deadly and cause spread to need adequate precautions to be undertaken for caregivers. This is not done to a large extent resulting in constant anger emerging in the laborer's minds. Sudan is witnessing severe drug abuse threats due to inappropriate training given to the doctors. "The current share of local manufacturing in the production of essential medicines in Sudan is only 5% (Who.int, 2021). It is observed that a large number of local pharmaceutical factories have stopped operating due to limited access to raw materials (Lucero-Prisno et al. 2020). According to the data from the Ministry of Trade and Industry, it has been seen that out of the 27 pharmaceutical factories in Sudan that cover 45% of the country’s consumption, only 19 factories are operating at half the production capacity (Who.int, 2021)”. All these factors also contribute to the inadequacy of healthcare. Labor market shortage is also fueled by the covid-19 pandemic situation. “November 2016, the previous Sudanese government implemented new policies which have led to the significant rise in the price of drugs (Who.int, 2021)". This is also related to inflation. The inflation rates are higher since Sudan depends on imported drugs and needs to find the process of healthcare adequacy. The crisis has become worse with the healthcare professionals not being given enough supplies to protect themselves from this menace (El-Sadig et al. 2021).
Local manufacturing of medicines is facing several quality issues. Essential commodity shortage and unavailability of raw material could fuel the scarcity of medicines. In a widespread non-governmental resource organization, the blame of the poor healthcare system is imposed on poverty and lack of supervision. Even though the government has come up with several service desks, the lack of awareness has prevented many of the population from fetching help for themselves. Pharmacies in the capital of Sudan Khartoum are running out of supply making it difficult for the caregivers (Ebaidalla, and Ali, 2019). With covid onboard the skilled laborers belonging to different industries are not able to manage a job and a stable income. This contributes to the lack of funding and not being able to afford healthcare. Transitional government and scarcity of financial resources are making the situation worse. People find it difficult to run their household and how they are supposed to be managing healthcare with large expenses.
Essential consumer goods are being out of reach of the commoner. Now, whatever, trained resources of healthcare are there, that might not get enough of the prices of their work which allows them to leave the job in the government sector and move towards the private sector. “Historically, drug importation and manufacturing problems have always been related to the decline in the local currency relative to the United States Dollar in Sudan (worldbank.org, 2021)”. This needs to be stopped and kept on affecting the distribution chains. The lack of government funding is not helping develop the medical reformation and create subsidiaries of the healthcare system that will provide free treatment to people. The current scenario is not following any healthcare distribution or a framework that manages healthcare. Businesses are thriving in terms of managing the scarcity of hard currency. One of the main drawbacks is found as “a lack of a blueprint from the government in developing the pharmaceutical sector. Corruption and bad governance also contribute to this bleak scenario (Ebrahim et al. 2017)". All caregivers are not gaining equal opportunity to become trained professionals and this leads to a wastage of resources and aiding to the corruption.
Lack of payments to the nurses and doctors are causing a threat to them for non-listening to the authority or cooperating in their respective jobs. There is a huge difference in payment for government and private hospitals which becomes a reason for this chaos. There are also gender pay gaps observed as a part of non-cooperation to the work in urban areas. A huge factor in managing the pay gaps is essential in monitoring the health care framework. Some of the frameworks allow focusing on ensuring the lives of caregivers which are not in use currently for the users and need to be implemented (Salim, and Hamed, 2018). Moreover, the lack of price control derecognizes the Sudan healthcare system and the origination of drug components.
4. Exploring options of reformation
Options for reformation are associated with generating insurance models that cover people with adequate support and services. The wrong deed is an unequal distribution of pay and no framework of operation as identified in previous sections. South Sudan reformation strengthened primary healthcare fragile settings in terms of managing the conflicts in higher authorities relating to healthcare (Sarriot et al. 2021). In previous statistics, the government funding was seen to be quite commendable in South Sudan healthcare however, after the pandemic situation the lowering of government health finance is now at less than 2% of the national budget that fuels the out-of-pocket spending and increases up to 54% of health expenditure (worldbank.org, 2021). “A shorter-term Health Systems Stabilization and Recovery Plan for the period 2020–2022 is intended to catalyze rebuilding the country's health system (Who. int, 2021)”. Acceleration of HSSP focuses on the priority interventions for giving training to the resource information systems. The government has now been focusing on a PHC accelerator that agrees to act as a representative of GAP agencies at global levels and create appropriate healthcare models (Omer, 2018).
The main elements of the strategy are identified to be including national authorities. It identifies as a balanced approach with aid to the resources and being familiar with the elements of planned and implemented concepts. Addressing the drawbacks of the system which needs reforming is done. The preparation of reconstruction needs the policymakers to pursue a vision of a lean, equitable, and effective health sector. Prioritization of preparedness response to the exploitation of threats and humanitarian development of components. There exist WHO roles to be implemented within each step of healthcare taken. All people working hardship have to scale up the relief camps and activities (Kheder, Awad, and Hamid, 2020). These small initiatives can contribute to the development of the enhanced charity. Decentralizing is a common form of managing the finance across the healthcare system and planning the sustainable expansion of equity. "The envisaged strategy will require a U-turn for WHO from the traditional disease control focus towards a more system-wide and long-term approach (Hassan, Tudor, T. and Vaccari, 2018)".
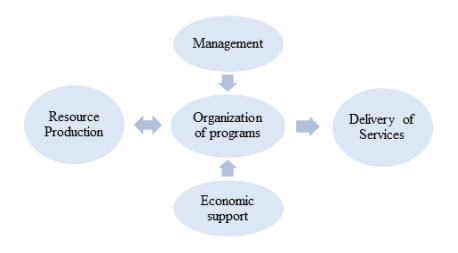
A suggested model will be the Reomer model of healthcare that is shown in image. Preserving local health by implementing drone technology on monitoring camps overhead. Remote healthcare will be progressed by using Skype chats and video calls with experts from the city to rural areas. Pregnant ladies and coronary patients will be given monitoring wearable devices to keep track of their healthcare activities (Lucero-Prisno et al. 2020). Strategic coordinates have been effective since using technology to real-time monitoring results in an error-free evaluation of patients. Using big data is going to help in the advanced analytical study of patients and error-free readings are expected to be taken that are going to save lives. Healthcare waste management and disposal also is associated within the reformation polices (Hassan, Tudor, and Vaccari, 2018).

References
Journals
Adwok, J., Eyobo, M., Achut, V. and Othomb, B., 2019. Regulatory challenges in a complex emergency environment: An update on South Sudan. South Sudan Medical Journal, 12(1), pp.21-23.
Bilali, B., 2020. State Fragility and Human Security Challenges in South Sudan. Analytical Politics, 1(1), pp.35-48.
Ebaidalla, E.M. and Ali, M.E.M., 2019. Determinants and impact of household's out-of-pocket healthcare expenditure in Sudan: evidence from urban and rural population. Middle East Development Journal, 11(2), pp.181-198.
Ebrahim, E.M., Ghebrehiwot, L., Abdalgfar, T. and Juni, M.H., 2017. Health care system in Sudan: review and analysis of strength, weakness, opportunity, and threats (SWOT analysis). Sudan journal of medical sciences, 12(3), pp.133-150.
El-Sadig, S.M., Fahal, L.A., Abdelrahim, Z.B., Ahmed, E.S., Mohamed, N.S. and Siddig, E.E., 2021. Impact of COVID-19 on doctors and healthcare providers during the pandemic in Sudan. Transactions of The Royal Society of Tropical Medicine and Hygiene, 115(6), pp.577-578.\
Hassan, A.A., Tudor, T. and Vaccari, M., 2018. Healthcare waste management: A case study from Sudan. Environments, 5(8), p.89.
Kheder, S.I., Awad, M.M. and Hamid, K., 2020. Prioritization of medicine importation by the private sector in Sudan: evidence from a data analysis, 2012-2015. Value in Health Regional Issues, 22, pp.27-34.
Lohiniva, A.L., Elwali, E., Abuobaida, D., Abdulrahim, A., Bukuluki, P. and Talaat, M., 2021. A theory-based exploration of antibiotic use in primary healthcare in Gezira state, Sudan. Implementation Science Communications, 2(1), pp.1-13.
Lucero-Prisno III, D.E., Elhadi, Y.A.M., Modber, M.A.A., Musa, M.B., Mohammed, S.E.E., Hassan, K.F., Dafallah, A., Lin, X., Ahmadi, A., Adeyemi, S. and Ekpenyong, A., 2020. Drug shortage crisis in Sudan in times of COVID-19. Public Health in Practice, 1, p.100060.
Omer, A.M., 2018. The efficiency of inefficiency: medicine distribution in Sudan. Universal Journal of Pharmaceutical Research, 3(2), pp.47-57.
Salim, A.M.A. and Hamed, F.H.M., 2018. Exploring health insurance services in Sudan from the perspectives of insurers. SAGE open medicine, 6, p.2050312117752298.
Sarriot, E., Olivas, E., Khalsa, S., Ashraf, S., Hejna, E., Hinds, G. and Story, W.T., 2021. Health systems effects of successive emergency health and nutrition projects: an embedded retrospective case study analysis in Sudan and Pakistan. Health Policy and Planning, 36(2), pp.176-186.
Lucero-Prisno III, D.E., Elhadi, Y.A.M., Modber, M.A.A., Musa, M.B., Mohammed, S.E.E., Hassan, K.F., Dafallah, A., Lin, X., Ahmadi, A., Adeyemi, S. and Ekpenyong, A., 2020. Public Health in Practice. Public Health, 1, p.100060.
Website
https://www.who.int/workforcealliance/countries/ssd/en/
https://www.worldbank.org/en/news/press-release/2020/09/30/world-bank-group-provides-support-to-help-sudan-manage-the-health-and-economic-impacts-of-the-covid-19
Continue your journey with our comprehensive guide to Analyzing Drug Overdose Deaths.
- 24/7 Customer Support
- 100% Customer Satisfaction
- No Privacy Violation
- Quick Services
- Subject Experts



